Fillings
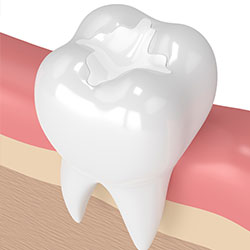 Traditional dental restoratives, or fillings, are most often made of silver amalgam. The strength and durability of this traditional dental material makes it useful for situations where restored teeth must withstand extreme forces that result from chewing, often in the back of the mouth.
Traditional dental restoratives, or fillings, are most often made of silver amalgam. The strength and durability of this traditional dental material makes it useful for situations where restored teeth must withstand extreme forces that result from chewing, often in the back of the mouth.
Newer dental fillings include ceramic and plastic compounds that mimic the appearance of natural teeth. These compounds, often called composite resins, are usually used on the front teeth where a natural appearance is important, but they can also be used on the back teeth depending on the location and extent of the tooth decay.
There are two different kinds of fillings: direct and indirect. Direct fillings are fillings placed into a prepared cavity in a single visit. They include silver amalgam, glass ionomers, resin ionomers, and composite (resin) fillings. Indirect fillings generally require two or more visits. They include inlays, onlays, and veneers. They are used when a tooth has too much damage to support a filling but not enough to necessitate a crown.
Wisdom Teeth
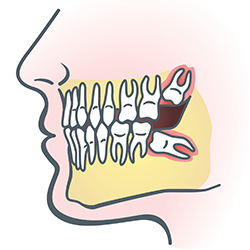 Wisdom teeth are types of molars found in the very back of your mouth. They usually appear in the late teens or early twenties, but may become impacted (fail to erupt) due to lack of room in the jaw or angle of entry. When a wisdom tooth is impacted, it may need to be removed. If it is not removed, you may develop gum tenderness, swelling, or even severe pain. Impacted wisdom teeth that are partially or fully erupted tend to be quite difficult to clean and are susceptible to tooth decay, recurring infections, and even gum disease.
Wisdom teeth are types of molars found in the very back of your mouth. They usually appear in the late teens or early twenties, but may become impacted (fail to erupt) due to lack of room in the jaw or angle of entry. When a wisdom tooth is impacted, it may need to be removed. If it is not removed, you may develop gum tenderness, swelling, or even severe pain. Impacted wisdom teeth that are partially or fully erupted tend to be quite difficult to clean and are susceptible to tooth decay, recurring infections, and even gum disease.
Wisdom teeth are typically removed in the late teens or early twenties because there is a greater chance that the teeth’s roots have not fully formed and the bone surrounding the teeth is less dense. These two factors can make extraction easier as well as shorten the recovery time.
In order to remove a wisdom tooth, your dentist first needs to numb the area around the tooth with a local anesthetic. Since the impacted tooth may still be under the gums and embedded in your jaw bone, your dentist will need to remove a portion of the covering bone to extract the tooth. In order to minimize the amount of bone that is removed with the tooth, your dentist will often “section” your wisdom tooth so that each piece can be removed through a small opening in the bone. Once your wisdom teeth have been extracted, the healing process begins. Depending on the degree of difficulty related to the extraction, healing time varies. Your dentist will share with you what to expect and provide instructions for a comfortable, efficient healing process.
Temporomandibular Disorder (TMD)
Millions of Americans suffer from chronic facial and neck pain as well as recurring headaches. In some cases, this pain is due to Temporomandibular Disorder, or TMD.
Your temporomandibular joints (TMJ) connect your lower jawbone to your skull. These joints get a lot of use throughout the day as you speak, chew, swallow, and yawn. Pain in and around these joints can be unpleasant and may even restrict movement.
Symptoms of TMD include:
- Pain in the jaw area
- Pain, ringing, or stuffiness in the ears
- Frequent headaches or neck aches
- Clicking or popping sound when the jaw moves
- Swelling on the sides of the face
- Muscle spasms in the jaw area
- A change in the alignment of top and bottom teeth
- Locked jaw or limited opening of the mouth
Should you notice any of these symptoms, let your doctor know. Your dentist can help indicate the presence of TMD and create an effective treatment just for you. There are a few simple steps you can take at home or work to prevent TMD from becoming more severe, or to prevent it from occurring:
- Relax your face — remember the rule: "Lips together, teeth apart"
- Avoid grinding your teeth
- Avoid constant gum chewing
- Don't cradle the phone receiver between your head and shoulder — either use a headset or hold the receiver in your hand
- Chew food evenly on both sides of your mouth
- Do not sit with your chin rested on your hand
- Practice good posture — keep your head up, back straight, and shoulders squared
Sleep apnea
Sleep apnea is a condition in which your breathing stops periodically during sleep, as many as 20-30 times per hour. Each time you stop breathing in your sleep, the resulting lack of oxygen alerts your brain, which temporarily wakes you up to restart proper breathing. Since the time spent awake is so brief, most people with sleep apnea don't remember it, and many believe they are getting a good night's sleep when, in fact, they are not. The constant wake-sleep, wake-sleep cycle prevents those with sleep apnea from achieving deep sleep, resulting in a constant drowsy feeling during the day.
What are the signs of sleep apnea?
The following symptoms can indicate the presence of sleep apnea. If you notice one or more of these, contact our practice.
- Insomnia or difficulty sleeping
- Loud snoring at night
- Waking up at night short of breath
- Snorting or choking sounds during the night (indicating a restart of breathing)
- Headaches upon waking in the morning
- Falling asleep unintentionally during the day
- Extreme drowsiness throughout the day
Are there different types of sleep apnea?
There are three categories of sleep apnea. The most common is called obstructive sleep apnea (OSA), and occurs due to a physical blockage, usually the collapsing of the soft tissue in the back of the throat. Less common is central sleep apnea (CSA), in which breathing stops because the muscles involved don't receive the proper signal from the brain. And some people suffer from "mixed" or "complex" sleep apnea, which is a combination of obstructive and central.
What are risk factors for sleep apnea?
Obstructive sleep apnea is more common in males than females, and more common in older adults (40+) than younger adults and children. However, anyone — regardless of gender or age — can suffer from sleep apnea. Other risk factors include obesity, smoking, drinking, use of sedatives or tranquilizers, and family history. Central sleep apnea strikes most often in people with heart disorders, neuromuscular disorders, strokes, or brain tumors.
How is sleep apnea treated?
Treatments for sleep apnea depend on the severity of each individual case, and the type of apnea. Basic treatment can be behavioral — for instance, patients are instructed to lose weight, stop smoking, or sleep on their sides instead of on their backs. Beyond that, oral devices can be used to position the mouth in such a way that prevents throat blockage. In more severe cases, surgery may be the best option.